Measles outbreak
Utah measles outbreak response
Total number of Utah residents who have been diagnosed with measles in this outbreak: 679
Total number of Utah residents who have been diagnosed with measles in this outbreak: 679
Number of Utah residents diagnosed with measles in 2026 to date: 482
Number diagnosed in 2025: 197
Number of Utah residents with measles reported to public health in the last 3 weeks: 8
Updated every weekday by 3:00 PM.
Last updated September 15, 2025.
Number of Utah residents diagnosed with measles in 2026 to date:
482
Number diagnosed in 2025:
197
Number of Utah residents with measles reported to public health in the last 3 weeks: 8
Counts are updated every Tuesday by 3:00 p.m. Last updated June 9, 2026.
Updated every weekday by 3:00 PM.
Last updated September 15, 2025.
Utahns diagnosed with measles by local health district

Wastewater dashboard
When measles is detected in wastewater it means one or more people in or traveling through that area has been infected with measles and is shedding the virus. Wastewater test results can tell us when the measles virus is in the wastewater, but the results don’t tell us how many people in the area are shedding the virus. It could be one person, or it could be multiple people.

Counts are updated every Tuesday by 3:00 p.m.
Last updated June 9, 2026.
Exposure locations
As cases are reported, public health officials in Utah investigate to identify individuals who are at risk of infection and any locations where possible exposures may have occurred. These exposure locations are listed by county below.
If you were at any of these locations during the time period listed, watch for measles-like symptoms and tap the button below to fill out an anonymous survey for information and next steps based on your risk for getting measles. The survey is available in both English and Spanish.
The Utah Department of Health and Human Services (Utah DHHS) wants to better understand the risk of measles spread in clinics and hospitals. Someone from Utah DHHS may contact you if you were exposed at a clinic or hospital to check if you got sick with measles after your exposure. We encourage you to answer the call or text and help us protect the health of Utahns. If you believe you got measles because of an exposure at a clinic or hospital, call us at (385) 515-5242.
Note about exposure locations on this website
The list below includes the exposure locations that have been reported to the Utah Department of Health and Human Services. Because measles is spreading in Utah, there may be other exposures or exposure locations that we are unaware of and are not listed here. As soon as a new exposure location is confirmed, we add it to the list below. The list is updated throughout the week. If you have questions about any of the exposure locations, contact your local health department.
Measles virus can remain in the air for up to 2 hours after a person with measles has visited a location. The times listed below account for that window. If you were at a location before or after the time and date listed for that location, you are not considered exposed.
Even if you have not had a confirmed exposure, if you think you may have been around someone with measles, watch for measles symptoms until 21 days have passed since you were around that person.
Exposure locations by county
As cases are reported, public health officials in Utah investigate to identify individuals who are at risk of infection and any locations where possible exposures may have occurred. These exposure locations are listed by county below. If you would like to see the exposure locations in a certain county, click that county’s name and the exposure locations will appear as a drop-down list.
If you were at any of these locations during the time period listed, watch for measles-like symptoms and click the button below to fill out an anonymous survey for information and next steps based on your risk for getting measles. The survey is available in both English and Spanish.
The Utah Department of Health and Human Services (Utah DHHS) wants to better understand the risk of measles spread in clinics and hospitals. Someone from Utah DHHS may contact you if you were exposed at a clinic or hospital to check if you got sick with measles after your exposure. We encourage you to answer the call or text and help us protect the health of Utahns. If you believe you got measles because of an exposure at a clinic or hospital, call us at (385) 515-5242.
Note about exposure locations on this website
The list below includes the exposure locations that have been reported to the Utah Department of Health and Human Services. Because measles is spreading in Utah, there may be other exposures or exposure locations that we are unaware of and are not listed here. As soon as a new exposure location is confirmed, we add it to the list below. The list is updated throughout the week. If you have questions about any of the exposure locations, contact your local health department.
Measles virus can remain in the air for up to 2 hours after a person with measles has visited a location. The times listed below account for that window. If you were at a location before or after the time and date listed for that location, you are not considered exposed.
Even if you have not had a confirmed exposure, if you think you may have been around someone with measles, watch for measles symptoms until 21 days have passed since you were around that person.
Exposure locations by county
As of June 9, 2026 there are no known measles exposure locations in Utah.
Utah measles dashboard

Wastewater dashboard
Frequently asked questions
Measles symptoms typically appear 7 to 14 days after exposure. People who have a high fever (101°F (38.3°C) or higher) and a cough, runny nose, or red eyes may have early stages of measles. A rash will usually appear after 4 days of fever. If you do develop symptoms you should stay away from other people and call a healthcare provider. Call first before you go to a clinic or hospital so they can prepare for your arrival and prevent other people from exposure.
We strongly encourage parents to talk to their healthcare provider about getting an early MMR vaccine for their children, even if they have not been exposed to someone with measles.
Should your infant younger than 12 months old get an early, extra dose?
Because measles is spreading throughout Utah, we suggest you talk to a healthcare provider about giving your infant an early, extra dose of the MMR vaccine if they are older than 6 months and younger than 12 months old.
It is a standard recommendation that infants 6–11 months old get an early, extra dose if they are traveling internationally or to an area where measles is spreading. Given the high levels of measles in Utah it is now appropriate to consider this early, extra for all Utah infants of this age.
Any infant who gets a dose before 12 months old will need to get 2 later doses in accordance with the standard vaccination schedule at 12–15 months and then a dose at 4–6 years.
Should your child 12 months or older get their second dose before the age of 4?
Young children can get their second MMR dose before 4 years old. The protection after 1 dose is very good. However, getting the second dose before the age of 4 is completely appropriate and fully protective, as long as they are older than 12 months and it has been at least 28 days since their first dose. Parents should discuss this option with their healthcare provider.
Two doses of the MMR vaccine provide lifelong protection against measles and you do not need a booster. If you or your child have not had 2 doses of the MMR or MMRV vaccine, we suggest you talk with a healthcare provider about getting vaccinated.
Special considerations:
- Before 1990, only 1 dose of MMR was recommended. If you were vaccinated before 1990 you may not have received your second dose. Talk with a healthcare provider about getting your second dose.
- Some people who were vaccinated between the years 1963 and 1967 got a less effective vaccine, which means they can still get measles. Anyone who got this vaccine is considered unvaccinated. Talk to a healthcare provider about whether you should get revaccinated if you were vaccinated between 1963 and 1967.
- If you were born before 1957, you likely do not need the MMR since we assume you were infected with measles in the past.
We recommend everyone make sure you are protected against measles. Talk to a healthcare provider if you have questions about whether you are protected against measles.
Most states look at how many kindergarten students have an exemption for the measles vaccine to measure measles vaccination rates.
During the 2025/2026 school year:
- 12% of in-person kindergarten students in Utah had an exemption for the MMR vaccine or were missing documentation to show they were vaccinated against measles.
- Nearly 12% of in-person kindergarten students in Utah had an exemption to any school-required vaccine.
- 12.7% of all students in Utah had an exemption to any school-required vaccine, including students in online schools.
You can look up the immunization coverage rates for children in Utah on the Utah Statistics page of the immunization program website. The immunization dashboard school vaccine exemption tab contains statewide and school-specific immunization data. You can also find reports that show trends in school vaccine exemptions for the past 10 years.
To avoid the chance of measles infection for unvaccinated individuals we recommend the following:
- Surround yourself with other vaccinated persons, especially in your household, if possible.
- If you’re exposed to someone who has the measles, talk to a doctor about post-exposure vaccination or medication.
- Avoid large gatherings and crowded places in areas with known outbreaks and ongoing transmission.
- Consider getting the MMR vaccine at least 1 month before you try to get pregnant, to avoid harm to your baby during pregnancy.
- Stay away from others if they are sick.
If you think you or your child may have measles, we recommend you:
- Stay home and away from others as much as possible.
- Seek care if you have a hard time breathing and/or fever won’t come down.
- Call the clinic or provider ahead of time and let them know you are concerned about measles; this is to protect other people from getting exposed in the waiting area, such as pregnant women and babies.
Information about breakthrough infections in Utah
A breakthrough measles infection happens when someone is vaccinated (they have had at least 1 MMR vaccine) and still gets measles after being exposed to the virus. Typically, people who get breakthrough measles usually have mild illness (lower fever, lighter rash, and fewer complications) and are less likely to spread the disease.
While the measles vaccine is very good at protecting people from getting sick with measles, it is not perfect. Most people who get the vaccine (97%) are well protected, but about 3% can get sick if they are exposed to the measles virus. During an outbreak, breakthrough infections are expected because high levels of the measles virus are circulating in the community. Two doses of the MMR vaccine are highly effective (97%) at preventing measles. Even a single dose is very effective (93%). It is rare to get a breakthrough infection if you’ve had 2 doses of the MMR vaccine.
Experts aren’t exactly sure why breakthrough infections happen. It could be that someone’s immune system did not fully respond to the vaccine. Breakthrough infections can also happen in people who have medical conditions or take medications that weaken their body so it cannot fight off the infection even when they have been vaccinated.
Breakthrough infections are more likely to happen in people who have only had 1 dose of the MMR vaccine.
If a vaccinated person gets measles, there are still benefits from the vaccine. Vaccinated people are less likely to have severe illness or have severe measles complications. They are also less likely to spread the virus to others.
Even though the MMR vaccine is very effective at preventing illness from measles, it is not 100% effective. This means we can still expect a small percentage of vaccinated people to get sick with measles after being exposed. For example, if 100 vaccinated people are exposed to measles, we can expect about 3 of them to get sick with measles (a breakthrough infection). If 200 vaccinated people are exposed, we can expect about 6 of them to get sick, and so on. This means that with an increasing number of vaccinated people being exposed, we end up with an increasing number of breakthrough infections.
Most people (more than 90%) in Utah have been vaccinated against measles. We believe many hundreds of vaccinated people in Utah have been exposed to measles during the current widespread outbreak. Even though hundreds of vaccinated people have likely been exposed, the vast majority of them have been protected by the vaccine and we only see the few where their body was not able to fight the virus off.
At the same time, a small proportion of Utahns have not been vaccinated. Those people are also being exposed to the virus. Unlike the vaccinated Utahns, a majority of the unvaccinated Utahns who are exposed to the virus will get sick with measles. This is why most of the people getting measles in Utah are unvaccinated even though they make up a small minority of our population.
Most people with 2 doses of the MMR vaccine are well protected, however the risk is not zero.
- It’s rare, but sometimes people who are fully vaccinated (have had 2 doses of the MMR vaccine) can still get infected if they are exposed. This means you should avoid contact with people who have measles (if possible).
- Breakthrough infections are more common when someone lives in a household, or has prolonged close contact, with someone who has measles.
- Adults with only 1 dose of MMR are still at risk for a mild case of measles.
Yes, it is still reasonable to watch for symptoms. While it is quite rare, it is possible for vaccinated people to get measles. If you have been exposed and experience measles-like symptoms, contact your local health department or a healthcare provider for further assessment and testing.
Currently, about 9.5% of confirmed measles cases are breakthrough cases. This is consistent with national data trends for areas experiencing a measles outbreak.
More information about measles
Measles resources
- Prepare for and respond to measles: Checklist for summer camps (PDF)
- Prepare for and respond to measles: Checklist for K–12 schools (PDF)
- Prepare for and respond to measles: A resource for K–12 schools (PDF)
- Prepare for and respond to measles: Checklist for early care and education centers (PDF)
- Prepare for and respond to measles: Checklist for businesses (PDF)
- Prepare for and respond to measles: A resource for businesses (PDF)
- Prepare for and respond to measles: A resource for shelters and congregate setting facilities
Measles overview
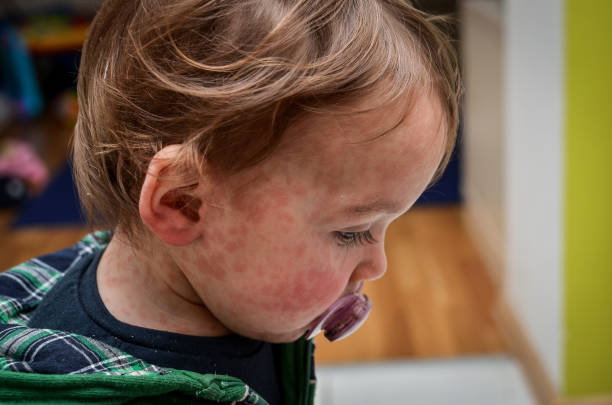
Symptoms
- High fever: Typically 101°F (38.3°C) or higher with:
- Cough
- Runny nose
- Red, watery eyes
- Rash (Measles rash usually begins as flat red spots on the face at the hairline. The spots then spread down to the neck, belly, arms, legs, and feet.)
Complications
- Pneumonia (a serious lung infection)
- Hospitalization
- Encephalitis or brain swelling (can cause cognitive disability, deafness, and seizures)
- Complications during pregnancy, such as the risk of premature labor (having your baby early), miscarriage, and your baby having a low birth weight
- Seizures
- Weakened immune system that can last weeks to years (increases the risk of bacterial infection and infection from other diseases)
- Death
When symptoms usually start (onset)
The first symptoms of measles start between 1 and 3 weeks after you are infected with the virus. Most people have symptoms at about 2 weeks.
How long it lasts (duration)
The first symptoms (fever, cough, runny nose, watery eyes) last for about 2 to 4 days but can be as short as 1 day or as long as 8 days.
The rash normally lasts 5 to 7 days and begins about 3 to 5 days after the first symptoms start.
Causes
Measles virus
How to prevent measles
- 2 doses of the MMR vaccine (measles, mumps, rubella), or
- 2 doses of the MMRV vaccine (measles, mumps, rubella, varicella)
Treatment
There's no specific treatment for a measles infection once it occurs. Treatment includes providing comfort measures to relieve symptoms, such as rest, and treating or preventing complications.
Frequently asked questions
Measles symptoms typically appear 7 to 14 days after exposure. People who have a high fever (101°F (38.3°C) or higher) and a cough, runny nose, or red eyes may have early stages of measles. A rash will usually appear after 4 days of fever. If you do develop symptoms you should stay away from other people and call a healthcare provider. Call first before you go to a clinic or hospital so they can prepare for your arrival and prevent other people from exposure.
We strongly encourage parents to talk to their healthcare provider about getting an early MMR vaccine for their children, even if they have not been exposed to someone with measles.
Should your infant younger than 12 months old get an early, extra dose?
Because measles is spreading throughout Utah, we suggest you talk to a healthcare provider about giving your infant an early, extra dose of the MMR vaccine if they are older than 6 months and younger than 12 months old.
It is a standard recommendation that infants 6–11 months old get an early, extra dose if they are traveling internationally or to an area where measles is spreading. Given the high levels of measles in Utah it is now appropriate to consider this early, extra for all Utah infants of this age.
Any infant who gets a dose before 12 months old will need to get 2 later doses in accordance with the standard vaccination schedule at 12–15 months and then a dose at 4–6 years.
Should your child 12 months or older get their second dose before the age of 4?
Young children can get their second MMR dose before 4 years old. The protection after 1 dose is very good. However, getting the second dose before the age of 4 is completely appropriate and fully protective, as long as they are older than 12 months and it has been at least 28 days since their first dose. Parents should discuss this option with their healthcare provider.
Two doses of the MMR vaccine provide lifelong protection against measles and you do not need a booster. If you or your child have not had 2 doses of the MMR or MMRV vaccine, we suggest you talk with a healthcare provider about getting vaccinated.
Special considerations:
- Before 1990, only 1 dose of MMR was recommended. If you were vaccinated before 1990 you may not have received your second dose. Talk with a healthcare provider about getting your second dose.
- Some people who were vaccinated between the years 1963 and 1967 got a less effective vaccine, which means they can still get measles. Anyone who got this vaccine is considered unvaccinated. Talk to a healthcare provider about whether you should get revaccinated if you were vaccinated between 1963 and 1967.
- If you were born before 1957, you likely do not need the MMR since we assume you were infected with measles in the past.
We recommend everyone make sure you are protected against measles. Talk to a healthcare provider if you have questions about whether you are protected against measles.
Most states look at how many kindergarten students have an exemption for the measles vaccine to measure measles vaccination rates.
During the 2025/2026 school year:
- 12% of in-person kindergarten students in Utah had an exemption for the MMR vaccine or were missing documentation to show they were vaccinated against measles.
- Nearly 12% of in-person kindergarten students in Utah had an exemption to any school-required vaccine.
- 12.7% of all students in Utah had an exemption to any school-required vaccine, including students in online schools.
You can look up the immunization coverage rates for children in Utah on the Utah Statistics page of the immunization program website. The immunization dashboard school vaccine exemption tab contains statewide and school-specific immunization data. You can also find reports that show trends in school vaccine exemptions for the past 10 years.
To avoid the chance of measles infection for unvaccinated individuals we recommend the following:
- Surround yourself with other vaccinated persons, especially in your household, if possible.
- If you’re exposed to someone who has the measles, talk to a doctor about post-exposure vaccination or medication.
- Avoid large gatherings and crowded places in areas with known outbreaks and ongoing transmission.
- Consider getting the MMR vaccine at least 1 month before you try to get pregnant, to avoid harm to your baby during pregnancy.
- Stay away from others if they are sick.
If you think you or your child may have measles, we recommend you:
- Stay home and away from others as much as possible.
- Seek care if you have a hard time breathing and/or fever won’t come down.
- Call the clinic or provider ahead of time and let them know you are concerned about measles; this is to protect other people from getting exposed in the waiting area, such as pregnant women and babies.
Information about breakthrough infections in Utah
A breakthrough measles infection happens when someone is vaccinated (they have had at least 1 MMR vaccine) and still gets measles after being exposed to the virus. Typically, people who get breakthrough measles usually have mild illness (lower fever, lighter rash, and fewer complications) and are less likely to spread the disease.
While the measles vaccine is very good at protecting people from getting sick with measles, it is not perfect. Most people who get the vaccine (97%) are well protected, but about 3% can get sick if they are exposed to the measles virus. During an outbreak, breakthrough infections are expected because high levels of the measles virus are circulating in the community. Two doses of the MMR vaccine are highly effective (97%) at preventing measles. Even a single dose is very effective (93%). It is rare to get a breakthrough infection if you’ve had 2 doses of the MMR vaccine.
Experts aren’t exactly sure why breakthrough infections happen. It could be that someone’s immune system did not fully respond to the vaccine. Breakthrough infections can also happen in people who have medical conditions or take medications that weaken their body so it cannot fight off the infection even when they have been vaccinated.
Breakthrough infections are more likely to happen in people who have only had 1 dose of the MMR vaccine.
If a vaccinated person gets measles, there are still benefits from the vaccine. Vaccinated people are less likely to have severe illness or have severe measles complications. They are also less likely to spread the virus to others.
Even though the MMR vaccine is very effective at preventing illness from measles, it is not 100% effective. This means we can still expect a small percentage of vaccinated people to get sick with measles after being exposed. For example, if 100 vaccinated people are exposed to measles, we can expect about 3 of them to get sick with measles (a breakthrough infection). If 200 vaccinated people are exposed, we can expect about 6 of them to get sick, and so on. This means that with an increasing number of vaccinated people being exposed, we end up with an increasing number of breakthrough infections.
Most people (more than 90%) in Utah have been vaccinated against measles. We believe many hundreds of vaccinated people in Utah have been exposed to measles during the current widespread outbreak. Even though hundreds of vaccinated people have likely been exposed, the vast majority of them have been protected by the vaccine and we only see the few where their body was not able to fight the virus off.
At the same time, a small proportion of Utahns have not been vaccinated. Those people are also being exposed to the virus. Unlike the vaccinated Utahns, a majority of the unvaccinated Utahns who are exposed to the virus will get sick with measles. This is why most of the people getting measles in Utah are unvaccinated even though they make up a small minority of our population.
Most people with 2 doses of the MMR vaccine are well protected, however the risk is not zero.
- It’s rare, but sometimes people who are fully vaccinated (have had 2 doses of the MMR vaccine) can still get infected if they are exposed. This means you should avoid contact with people who have measles (if possible).
- Breakthrough infections are more common when someone lives in a household, or has prolonged close contact, with someone who has measles.
- Adults with only 1 dose of MMR are still at risk for a mild case of measles.
Yes, it is still reasonable to watch for symptoms. While it is quite rare, it is possible for vaccinated people to get measles. If you have been exposed and experience measles-like symptoms, contact your local health department or a healthcare provider for further assessment and testing.
Currently, about 9.7% of confirmed measles cases are breakthrough cases. This is consistent with national data trends for areas experiencing a measles outbreak.
More information about measles
Measles resources
- Prepare for and respond to measles: Checklist for summer camps (PDF)
- Prepare for and respond to measles: Checklist for K–12 schools (PDF)
- Prepare for and respond to measles: A resource for K–12 schools (PDF)
- Prepare for and respond to measles: Checklist for early care and education centers (PDF)
- Prepare for and respond to measles: Checklist for businesses (PDF)
- Prepare for and respond to measles: A resource for businesses (PDF)
- Prepare for and respond to measles: A resource for shelters and congregate setting facilities